Our Community
Tina’s Story

When diabetes meets pancreatitis and suspected liver cancer…
This wonderful little 13-year-old lady, Tina, first met our Emergency + Critical Care and Internal Medicine teams following a build up of symptoms. Her local vet had already diagnosed Tina with diabetes, however over the course of a few months, she had started to become increasingly lethargic, and had developed soft faeces, excessive drinking, high temperature, abdominal distension and, most recently, vomiting.
Through investigations at The Ralph, her care team discovered more complexities. This is her story…
Tina’s main issues were that, despite treatment, her diabetes was unable to be controlled. She was also suffering from a hepatopathy (liver condition). Following an ultrasound scan and FNA (fine needle aspiration) sampling, our Internal Medicine team suspected that Tina may have diffuse hepatocellular carcinoma (a form of cancer spread throughout the liver).
We also found that there was some excess fluid in Tina’s abdominal cavity (peritoneal effusion), and analysis of this fluid hinted at previous bleeding episodes, raising further concerns about cancerous changes in her liver.
Inflammation from the suspected liver cancer could help explain Tina’s resistance to her insulin treatment and overall health decline. This was supported when our Internal Medicine team decided to give Tina some anti-inflammatory medication: her temperature normalised, she became brighter and her appetite improved.
Our clinicians fitted Tina with a FreeStyle Libre Continuous Glucose Monitoring (CGM) device. This is a sensor that sits on the skin, with a small flexible needle entering the tissues just below the surface, detecting the glucose concentration in the tissues. The devices are also used in human medicine, and allow you to simply scan the sensor with a smartphone and see an instant glucose reading. This spares our patients from frequent ear pricks with more traditional methods of blood glucose monitoring.
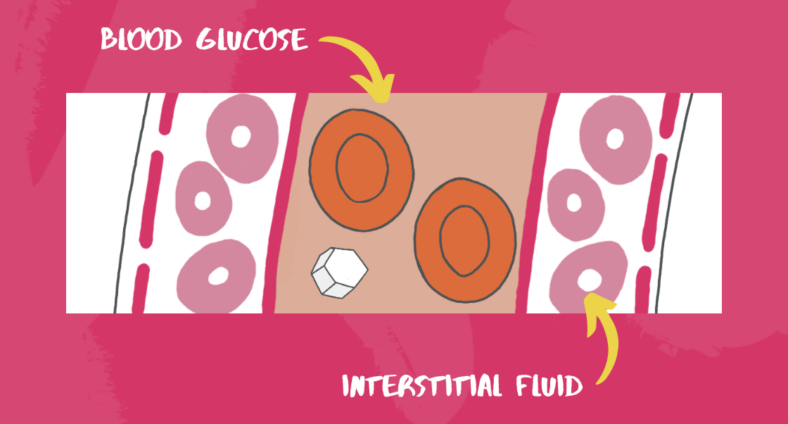
CGM devices work by measuring the glucose concentration in the interstitial fluid (fluid surrounding the cells of the tissues), which is in an equilibrium with the glucose in the blood.
These readings meant that we were able to vary Tina’s insulin doses depending on her glucose levels. It can be very difficult to maintain stable glucose readings, but thanks to Tina’s dedicated carers, her diabetic control improved and could be continually managed at home.
A month later, Tina developed some diarrhoea and reduced appetite. Any change in diet can throw off the stabilised glucose levels, and so she returned to The Ralph. Our clinicians decided that again, an abdominal ultrasound was needed to determine the causes of Tina’s symptoms. This time, it led to a diagnosis of pancreatitis, which is the inflammation of the pancreas (a long, flat gland that’s tucked behind the stomach). It helps the body digest food and regulate blood sugar levels, which explains how its inflammation would affect Tina’s appetite and also her blood sugar control.

Months later, Tina returned, and this time the team unfortunately found that she was severely anaemic. Blood analysis revealed that she had a packed cell volume (PCV; the volume of red blood cells in the blood) of 18%, much below the ideal volume of 35-55%. This was suspected to be caused by hepatic bleeding (from her liver), both into the abdomen and cavities within the liver itself. She required an urgent blood transfusion to help replace the blood that she had lost through this bleeding, and despite a suspected reaction to the transfusion, Tina’s resilience shone through: her condition improved and she returned home when she was feeling better.
Due to the nature of Tina’s cancer, the care she is receiving is palliative. We are treating her with medication to help reduce the bleeding from her liver, and keeping her diabetes stable with her insulin treatment. Her vibrant little character and lively interactions with our team always brighten our day, and we know she has a great life with her carer, filled with love.
One day at a time…

Tina getting excited for her walk!

Tina curled up on the sofa with her feline housemate, Misty
Thank you for reading Tina’s story. We post regular patient stories on our Instagram, Facebook and LinkedIn, so give us a follow for more patient and team content!
Take care,
Team Ralph 🐾
