Our Community
The Ralpher – September 2019 Edition
Hello!
Welcome to our penultimate edition of The Ralpher for the year. It’s jam-packed with all things Ralph including news, stories, and tips. We hear a couple of interesting ECC and Soft-Tissue Surgery tales from the clinical floor and some insightful physiotherapy tips to help your patients get back on their feet as soon as possible.
As always, we would love to hear from you. So, if you have a question, feedback, or a suggestion please drop us a line.
Take care,
Team Ralph
In this month’s edition…
Spotlight on Orthopaedics…
Meet our surgeons Alan and Stefano, and our first CUE patient Poppy
Tales from the clinical floor:
This month we hear about Maisie’s remarkable recovery, and Drusy’s sublingual swelling
Kim’s top physiotherapy tips:
How to get your patients back on their feet as quickly as possible
More information:
We share details on our October CPD event
Team announcements
We are super proud to announce Laura Jones, our Senior Medicine Nurse, passed her Veterinary Technician Specialist (VTS) exams this summer and is now a Veterinary Technician Specialist in Small Animal Internal Medicine. Laura is only 1 of 5 people currently in the UK to hold a VTS in Small Animal Internal Medicine.

Laura
The Veterinary Technician Specialty in Small Animal Internal Medicine is awarded by the Academy of Internal Medicine for Veterinary Technicians and accredited by the American Veterinary Association. The application to sit the exam alone took Laura hundreds of hours to complete, and included a total of 65 case logs and 4 case reports covering respiratory, haematological and urogenital medicine. It is highly competitive, with only a handful of applicants being successful to sit the exam.
Laura travelled to the American College of Veterinary Internal Medicine congress in Arizona to sit the exam – which took 4 hours to complete. It was a nerve-racking 6-week wait for the results, with a very positive outcome. Laura will be heading back to the US next year to attend her pinning ceremony at the congress in Baltimore.
Having worked so incredibly hard for both the application and the exams we are all so delighted of Laura’s achievements knowing they are richly deserved.
Spotlight on Orthopaedics
Despite the fact that around half the bones in cats and dogs’ bodies are in their paws, the most common areas treated by orthopaedic vets are knees and elbows.
In July, we introduced you to Alan Danielski who joined Team Ralph’s surgery team. He works alongside fellow Orthopaedic Surgeon Stefano Genoni to provide the highest level of orthopaedic care by combining years of collective experience with the latest, state of the art equipment.
The Ralph is one of a handful of veterinary centres in the country to offer canine unicompartmental elbow replacement (CUE) surgery. CUE aims to treat the most serious cases of osteoarthritis as a result of elbow dysplasia, and has an 80% long-term improvement rate. This month, Labrador Poppy Thomas became the first Ralph patient to undergo the major CUE operation to stop the bones rubbing in her right elbow. See pictures of the results below!
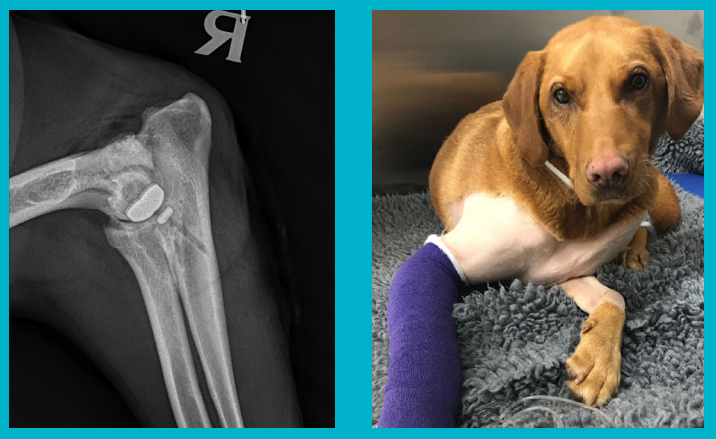
X-ray showing the partial resurfacing of the elbow and Poppy recovering post-op
Poppy will come back to us in a few months time to be radiographically reassessed.
Our Orthopaedic Service investigates an extensive range of musculoskeletal (bone, muscle, ligament and tendon) disorders, and we are passionate about providing a comprehensive, integrated and focused perioperative care plan for each patient.
We perform many other surgical treatment procedures at The Ralph, including: Proximal Abducting Ulnar osteotomy (PAUL); treatment of shoulder, elbow and stifle Osteochondritis Dissecans (OCD); cruciate ligament repair (lateral tibiofabella suture, TPLO, cranial closing wedge osteotomy); medial patella luxation repair; joint arthrodesis; angular limb deformity correction; arthroscopy; and repair of simple and complex fractures and joint dislocation.
Our dedicated and highly qualified surgical team utilise a range of specialist surgical and non-surgical equipment to support their delivery of excellent and compassionate care. This includes advanced diagnostic imaging, a Storz arthroscopy tower, a patellar groove replacement kit and a Biomedtrix total hip replacement kit.
Surgery goes hand in hand with post-operative physiotherapy and rehabilitation. Scroll down to read top tips for primary care practices from our Head of Physiotherapy & Rehabilitation, Kim Sheader.
Alan and Stefano are always happy to give general advice and discuss all things orthopaedic! Drop us a line: [email protected]
Tales from the clinical floor
Maisie
Maisie is a 7 year old female Domestic Long-haired cat who was referred to The Ralph’s Emergency and Critical Care (ECC) Service for evaluation of respiratory distress due to pleural effusion.
Maisie had a history of an acute onset of lethargy, anorexia for three days, and an acute and progressive increase in respiratory rate and effort for twenty-four hours before presentation. A chest radiograph was performed by her primary care practice and Maisie was found to have pleural effusion. The effusion was sampled and this was consistent with a septic exudate. Maisie was referred to The Ralph for further management and twenty four-hour monitoring.
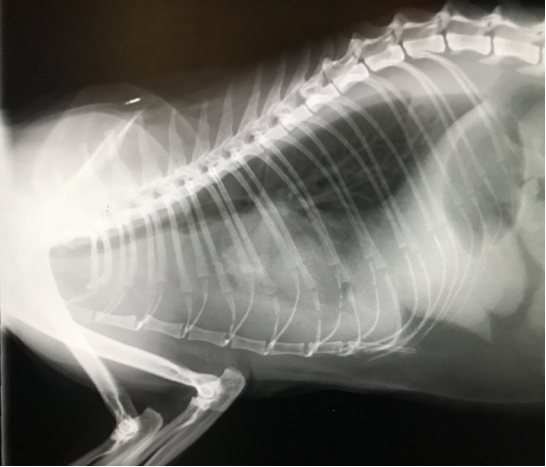
Referral radiograph showing significant pleural effusion causing retraction of the lungs
Upon admission, Maisie was in a critical state of septic shock. She had a severe increase in respiratory rate and effort, open mouth breathing, and hypoxaemia (oxygen saturation on admission was 80%). She was immediately placed in an oxygen cage to provide oxygen supplementation. However, her dyspnoea worsened significantly. Rapid induction and intubation was performed to facilitate drainage and prevent respiratory arrest. An over-the-wire Seldinger-style chest drain was placed in the right hemithorax and 210 ml of brown, foetid, flocculent fluid aspirated. Only a small amount of effusion was identified in the left hemithorax. Following pleural drainage, Maisie was saturating normally and she recovered slowly from the general anaesthesia.
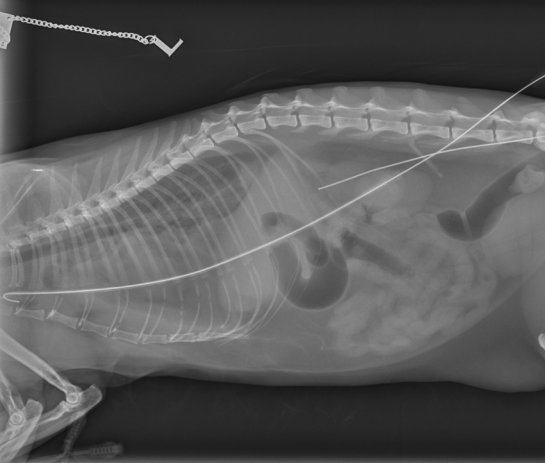
Radiograph taken during placement of chest drain. Wire confirms the appropriate location
Maisie was extremely critical in the first twenty four hours. She was started on intravenous broad-spectrum antibiotics (amoxicillin and clavulanic acid, and marbofloxacin). She was profoundly hypotensive despite repeated boluses of fluid therapy. A low rate infusion of noradrenaline was therefore started to which her blood pressure responded positively. Maisie was also hypoalbuminaemic and this, coupled with her need for fluid resuscitation, prompted a fresh frozen plasma transfusion. A naso-oesophageal tube was placed and enteral feeding was initiated when Maisie was more stable.
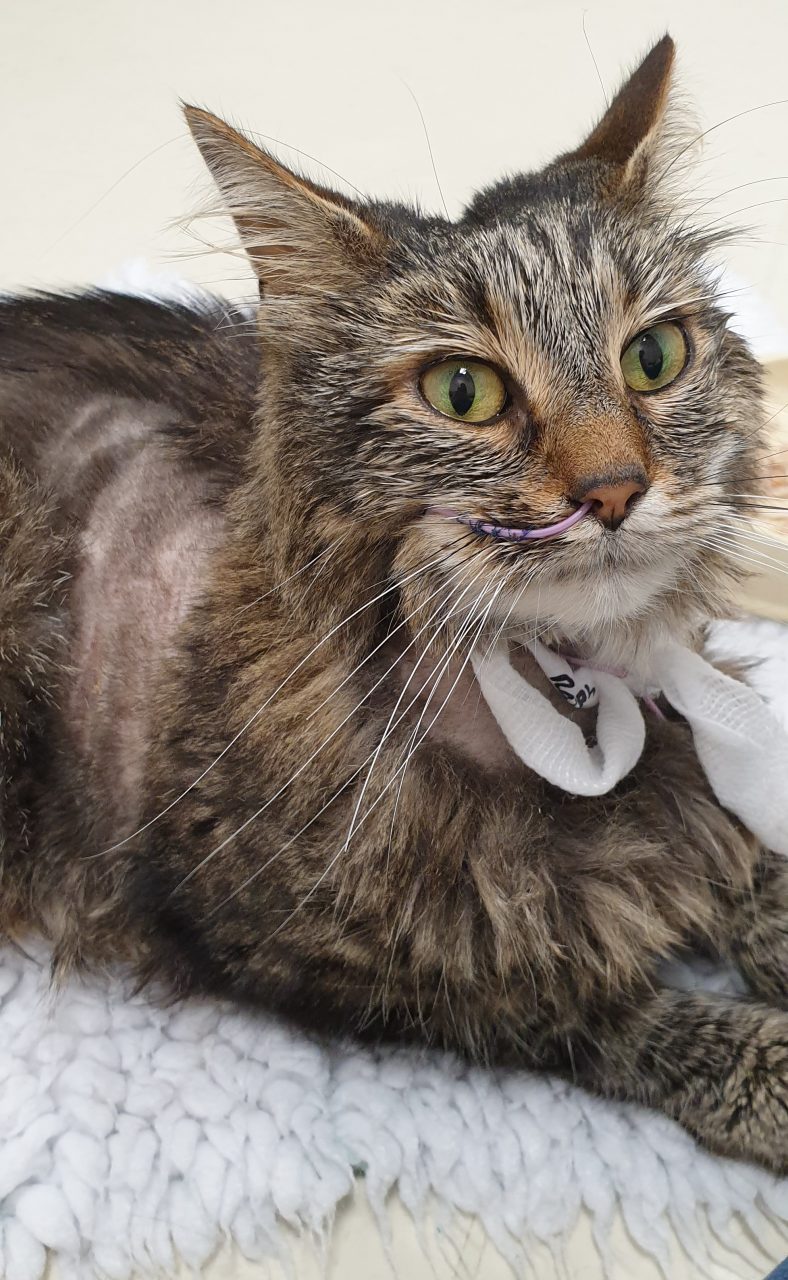
Maisie recovering in our Cat ICU
Throughout her stay, Maisie received regular chest drainage and lavage. Her respiratory status steadily improved and she was weaned of both vasopressor therapy and oxygen supplementation. Physiological doses of hydrocortisone were administered empirically in case of critical illness-related corticosteroid insufficiency (CIRCI). The consistency of the fluid improved every day and after five days her chest drain was removed. Maisie was discharged home with a course of antibiotics to continue treatment for at least 2 weeks.
Maisie at home
Maisie was diagnosed with pyothorax, an infection of the pleural space outside of the lungs and within the chest cavity. Because the fluid is so inflammatory, a fever is usually also present. In cats, a pyothorax usually starts as a bite wound. The bite may penetrate the chest cavity outright and deposit bacteria into the pleural space where abscessation occurs, or the bite may abscess externally but eventually rupture inward. In either case, the result is a bacterial infection in the pleural space and the formation of pus. Other causes of pyothorax include rupture of the oesophagus, migrating foreign body, bacterial pneumonia leading to rupture of a lung abscess, or lung parasites. Maisie’s carer identified a claw in her fur prior to admission, and perhaps in Maisie’s case it was this claw that could have acted as a source of infection.
Drusy
Drusy, an eight-year old neutered female Flat-coated Retriever, recently presented to The Ralph with a history of a right sublingual swelling. In addition, the carer reported that Drusy appeared to be salivating more. There was no dysphagia or dyspnoea.
On clinical examination Drusy was bright and alert. A moderate right sublingual swelling was evident, resulting in displacement of the tongue to the left. Thoracic auscultation and abdominal palpation were within normal limits. Haematology and biochemistry were unremarkable.
Drusy was anaesthetised. Examination of the oral cavity demonstrated a perforating wound on the caudal aspect of the right sublingual region. Exploration of the wound demonstrated fistulous tracts extending to the caudal retropharyngeal region. No foreign material was found. A CT scan with contrast of the head was performed which demonstrated a heterogenous, contrast enhancing mass lesion (yellow arrowheads), with numerous disorganised fluid-filled cavities and tracts, in the region of the right mandibular/sublingual salivary ducts and polystomatic sublingual salivary glands. A fine needle aspirate of the sublingual swelling was inconclusive.
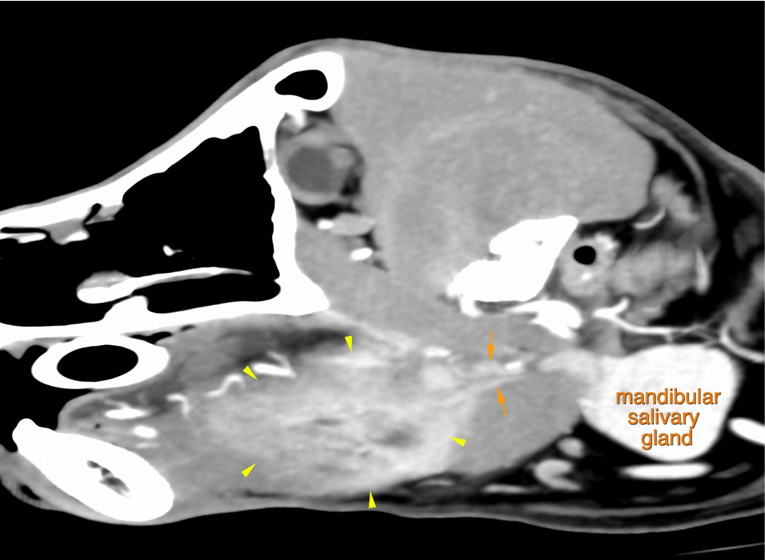
Mass lesion with fluid cavities ventral to the base of the tongue yellow arrowheads)
The differential diagnoses in this case included an oropharyngeal stick injury, sialadenitis, salivary mucocoele or neoplasia. Most salivary mucocoeles are of unknown cause ie. idiopathic. The sublingual wound and CT findings in Drusy’s case were unusual for an idiopathic salivary mucocoele. We suspected the cause of the sublingual swelling was a penetrating wound (stick injury) damaging the salivary ducts leading to leakage of saliva into the surrounding tissues.
Surgery is the treatment of choice for salivary mucocoeles. Whilst marsupialisation of the mucocoele can be performed, surgical excision of the affected salivary glands is recommended. A right mandibular/sublingual sialadenectomy was performed with a ventral approach. The mandibular/sublingual salivary glands and ducts were excised by tunnelling under the digastricus muscle to ensure complete removal of the salivary tissue. Histopathology confirmed chronic sialoadenitis. There was no evidence of neoplasia.
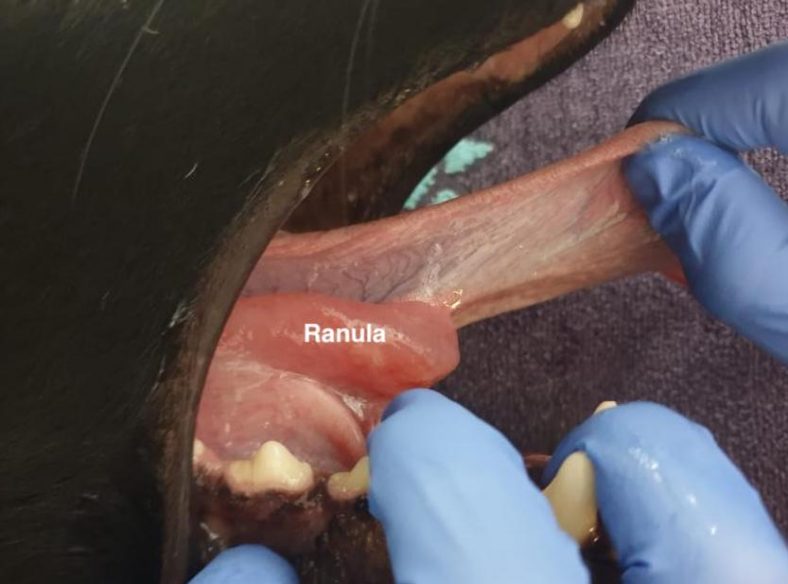
Drusy made an unremarkable recovery from surgery. She was hospitalised overnight and discharged to continue her recovery under the careful watch of her carer. At Drusy’s post-operative check, examination of the oral cavity demonstrated complete resolution of the ranula. The prognosis in this case is favourable and we would expect Drusy to make a full recovery.
The power of physiotherapy
Our Head of Physiotherapy and Rehabilitation, Kim Sheader MCSP HCPC ACPAT Cat A RAMP, shares her tips for how to make the most of physiotherapy and get patients back on their feet as quickly as possible.
1. Start physiotherapy sooner rather than later.
You don’t need to wait for six weeks crate rest to be over. Kim recommends referring patients for physiotherapy one week post-surgery, or diagnosis. This is particularly important for patients who have undergone orthopaedic surgery, or who have recently been diagnosed with a neurological condition. Whilst some people may be cautious to refer for physiotherapy before the patient has had six weeks cage rest, the sooner a patient can undergo physical therapy the better. Not only will it help strengthen the patient’s muscles, it also does wonders for their wellbeing whilst they are recuperating.
2. Physiotherapy is not just for dogs with arthritis
Cats can have physiotherapy too! Physiotherapy and hydrotherapy can help both canine and feline patients with multiple conditions – including orthopaedic, neurological, and respiratory conditions.
3. Physiotherapists can be very handy with a sewing machine
Kim can create custom-made neoprene supports and thermoplastic splints for patients – big and small! These splints and supports form part of the patient’s rehabilitation and can be used in both the short- and long-term.

Kim has been a Chartered Physiotherapist since 2000. She spent her first 10 years as a Physiotherapist treating humans, and then obtained her Post Graduate Diploma in Veterinary Physiotherapy at the Royal Veterinary College, London. Kim has worked as a Veterinary Physiotherapist at small animal referral hospitals for the past 7 years, also providing a mobile physiotherapy service to veterinary practices and pet carers.
As the Head of Physiotherapy and Rehabilitation, Kim is hands-on treating a variety of inpatients and outpatients. She is experienced in the use of laser therapy, physiotherapeutic techniques for a variety of problems, including balance, weakness, tonal changes and chronic pain, and hydrotherapy. Kim is passionate about contributing to the ongoing improvement of small animal physiotherapy care, and will be conducting research at The Ralph to support this.
To find out more about our Physiotherapy and Rehabilitation Service please click on the link or email Kim, [email protected]
CPD Corner
Our next free CPD evening will take place on Tuesday 15th October 2019. The session titled ‘Taking a closer look with Diagnostic Imaging’ will be presented by our Head of Diagnostic Imaging, Livia Benigni DVM MRCVS FHEA CertVDI PgCertAP DipECVDI. Livia will guide you through some challenging imaging cases and will provide a refresher on thoracic radiology. For more details and to register your attendance check out our events page.
Missed out on one of our previous CPD events?…Not to worry!
You can now watch recordings from our CPD sessions on our website. Videos and audio recordings will be available shortly after each live event, and are free to access. Just visit our new Library + Learning page to catch up on the event you missed.
Thank you for taking the time to read our news and stories from inside the hospital. Stay tuned for our next edition (the final one of the year!), and more news on our upcoming events.
Take care,
Team Ralph
